
Testosterone is the primary male sex hormone and an anabolic steroid that plays vital roles in men’s health. It drives masculine development at puberty, regulates muscle mass, bone density, red blood cell production, and libido, and affects mood and energy. Still, many younger and middle-aged men also experience deficiencies. Recently, interest in “low T” has surged: millions of men seek information and treatment. Clinicians note a three-fold rise in testosterone prescriptions in the U.S. over the past decade, as reported by JAMA Internal Medicine. At the same time, debate continues about who truly needs therapy. This guide will help you understand what testosterone is, how levels change through life, and how to recognize, diagnose, and treat low testosterone. You’ll learn common symptoms of hypogonadism, causes (including lifestyle factors), and evidence-based treatment options, from natural lifestyle fixes to medical therapies. We’ll also dispel myths (e.g., “TRT causes prostate cancer”) with facts, and answer key FAQs on testosterone and men’s health. Whether you’re health-conscious, facing fatigue or low libido, or just curious about “how testosterone works,” this guide aims to give you a thorough, up-to-date overview. In adult men, normal testosterone supports vitality: maintaining muscle mass, fat distribution, mood balance, and sexual function. For a detailed breakdown, see the benefits of high testosterone. Some signs of high levels may be subtle. Check our guide on recognizing elevated testosterone. Wondering about its effect on growth? Here's the science behind testosterone and height.
What is Testosterone?
Testosterone is an androgenic steroid hormone mainly produced in the male testes (and in much smaller amounts by the ovaries in women and adrenal glands in both sexes). As the body’s main male hormone, it stimulates the development of male characteristics: deepening the voice, facial and body hair, and growth of genitalia. It’s a lipid (fat)‑derived hormone built from cholesterol. In men, testosterone levels are much higher than in women.
The Hormone’s Roles
Testosterone has a wide range of functions: it promotes muscle and bone strength, supports red blood cell and sperm production, and sustains libido and a sense of well-being. For example, it signals the bone marrow to make new blood cells, keeps bones and muscles healthy, and enhances sexual desire. In fetal development, testosterone drives male sexual organ formation, and during puberty, it triggers the typical adolescent growth spurt and the development of pubic hair, deeper voice, and increased height. In adult men, normal testosterone supports vitality: maintaining muscle mass, fat distribution, mood balance, and sexual function. Like many hormones, testosterone levels fluctuate daily and seasonally. They are highest in the morning (which is why blood tests are done early). Although labs vary, young adult men typically have about 300–1,000 ng/dL (nanograms per deciliter). A common reference range is roughly 300–1,000 ng/dL for healthy adult males. Levels peak in late adolescence/early 20s and then slowly decline with age. Each year, after about age 30–40, men lose roughly 1–2% of their testosterone. In other words, “levels peak by early adulthood and drop up to 2% per year after age 40,” according to the Mayo Clinic.
Hormone Chemistry
Testosterone is classified as an anabolic-androgenic steroid. “Anabolic” refers to its muscle-building effects, while “androgenic” describes its role in developing male characteristics. Chemically, testosterone is derived from cholesterol. In the bloodstream, it circulates in two forms: bound (primarily to sex hormone–binding globulin or SHBG) and free (the active form).
Synthetic testosterone used in medical treatments is structurally identical to natural testosterone. However, it is often administered in higher doses, especially in performance-enhancing contexts. When athletes or bodybuilders use “steroids,” they are usually taking supraphysiologic doses of synthetic testosterone, which may carry serious health risks such as hormonal imbalances, cardiovascular strain, and infertility. For a full overview of these effects, see our blog on Testosterone Injections: Uses, Benefits, and Potential Side Effects.
Testosterone Across a Man’s Life
Testosterone levels fluctuate significantly throughout a man’s life, from puberty to old age. Understanding this natural rhythm can help you spot when something might be off or simply part of the aging process.
Puberty and Early Adulthood
Testosterone production ramps up during puberty, usually between the ages of 10 to 15. This surge triggers key developmental changes such as growth spurts, increased muscle and bone mass, pubic and underarm hair, genital growth, and voice deepening. Teenage testosterone levels vary greatly, moving from very low pre-puberty values to hundreds of nanograms per deciliter (ng/dL) during adolescence.
By the late teens and early 20s, most men reach peak testosterone, typically around 600–900 ng/dL. In general, men in their 20s have the highest average levels of testosterone. If you're interested in the typical hormone patterns across the lifespan, refer to our full guide on Testosterone Levels by Age.
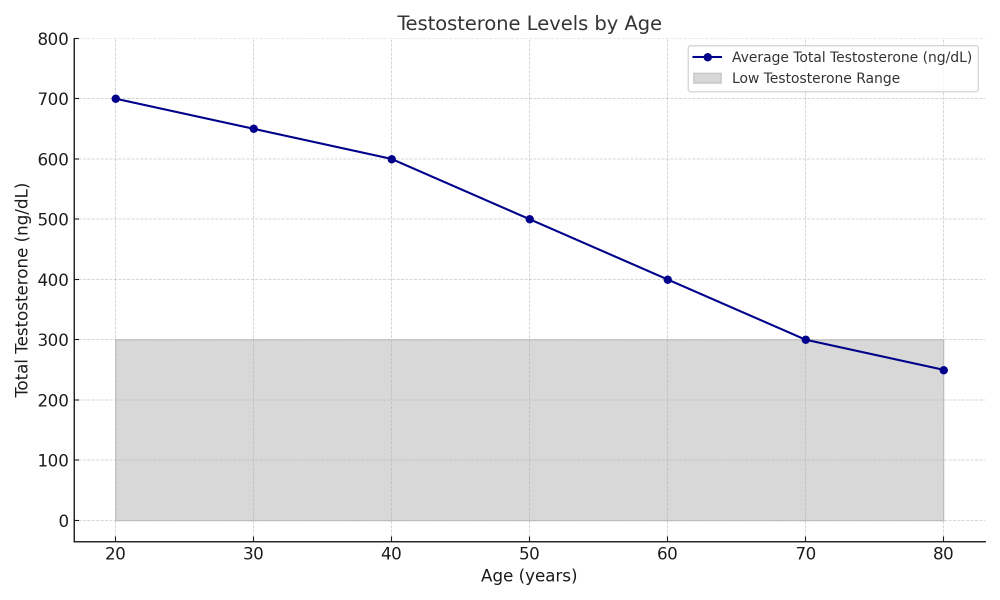
A large-scale study found that by age 45, nearly 40% of men may have testosterone levels classified as low. By age 80, that number rises to 50%, often due to age-related decline. For example, a healthy 20-year-old male might have 500–700 ng/dL, while a healthy man over 70 could average 150–300 ng/dL. That said, levels are only one part of the story; symptoms and health status matter, too. For more on what counts as “normal,” check out our article on Testosterone Levels in Men.
Middle Age
In your 30s and 40s, testosterone begins a slow, steady decline. On average, men lose about 1–2% of total testosterone per year after age 30. This can lead to subtle shifts in energy, mood, body composition, and libido. However, age isn’t the only factor. Health conditions like obesity or metabolic syndrome can accelerate the decline.
A Harvard health report notes that body weight may influence testosterone more than age. A 5-point increase in BMI (e.g., 30 to 35) can mimic the effects of a decade of aging. That means an overweight 40-year-old may have the testosterone profile of a healthy 50-year-old.
In terms of prevalence, about 12% of men in their 50s meet the clinical criteria for low testosterone (also called “biochemical hypogonadism”), rising to 49% in their 80s. But only 6% of men have both low levels and multiple symptoms such as fatigue, low libido, or mood changes. To learn more about how doctors diagnose and treat these symptoms, read our guide on Low Testosterone: Symptoms, Diagnosis, and Treatment.
Older Age
In men over 60, testosterone continues its downward trend. Even healthy older men often have levels below 400 ng/dL. Research shows that by age 70, many men fall into the 150–300 ng/dL range, nearly a third less than in early adulthood.
However, testosterone levels don’t tell the whole story. Some men function well with lower numbers, while others experience symptoms like low energy, erectile issues, or loss of muscle mass. It's important to consider both bloodwork and clinical symptoms before jumping to conclusions. For more on how aging affects sexual health specifically, see our article on Erection Problems on TRT: What to Know Before You Start Testosterone Therapy.
Despite the natural decline, not every man develops low testosterone symptoms. But when symptoms do appear alongside a significant drop in levels, doctors may diagnose late-onset hypogonadism, also known as “andropause.” Conditions like diabetes, chronic illness, and obesity can increase the risk of this age-related hormonal deficiency. To naturally support healthy hormone levels as you age, explore our tips in 8 Ways to Naturally Increase Testosterone.
Symptoms of Low Testosterone
Many symptoms of low testosterone (male hypogonadism) are subtle or overlap with other conditions. However, key signs tend to affect sexual function, body composition, and mood or energy. Men and doctors look for these red flags:
Sexual Dysfunction: A reduction in sex drive (libido) is a classic symptom. Men may have less interest in sexual activity. Low testosterone can also cause or worsen erectile dysfunction (difficulty getting or maintaining an erection). Some men with very low T experience smaller, softer testes. Fertility can decline testosterone deficiency often leads to decreased sperm count and infertility.
Changes in Body Composition: Low T tends to reduce muscle mass and strength while increasing body fat. Men may notice they put on fat more easily and lose muscle tone. Testosterone also influences bone density; long-standing low T can lead to osteoporosis (thinning bones) and higher fracture risk. Other physical changes can include decreased body and facial hair growth, and in some cases, swelling of breast tissue (gynecomastia).
Energy, Mood, and Cognition: Many men report that low testosterone causes fatigue and low energy. They may feel chronically tired without a clear reason. Mood changes are common. Low T is linked to feelings of sadness or depression and irritability. Cognitive effects include difficulty concentrating and “brain fog.” Other possible signs are anemia (low blood counts) and even hot flashes (similar to menopausal symptoms).
Other Signs: Decreased nighttime or early-morning erections, sleep disturbances, decreased motivation or confidence, and a general sense of not “feeling like yourself” can all accompany low T. Some men also notice trouble with spatial awareness or memory (though research on cognition is still evolving).
It’s important to note that many of these symptoms, such as nonspecific fatigue, moodiness, and weight gain, can result from stress, aging, medical conditions, or poor sleep, not just low testosterone. Likewise, not every man with low testosterone will have every symptom. The combination of several signs (especially sexual symptoms plus others) makes hypogonadism more likely. If you experience a cluster of these symptoms, consider discussing them with a doctor and getting your levels checked.
Causes of Low Testosterone
Low testosterone (hypogonadism) can arise from many factors, often divided into primary (testicular) and secondary (pituitary or hypothalamic) causes. In practice, common causes include:
Aging and Medical Conditions: By far the most common cause in adult men is age-related decline, sometimes called “late-onset hypogonadism.” Testosterone production naturally slows with age. This decline can be accelerated by chronic illnesses. For example, type 2 diabetes, obesity, and metabolic syndrome are strongly linked to lower testosterone. Experts note that weight gain itself has a bigger impact on T than aging. Even healthy middle-aged men often have lower T if their BMI is high. Other health conditions, such as sleep apnea, liver or kidney disease, HIV/AIDS, or thyroid disorders, can also suppress testosterone production.
Obesity and Lifestyle: Being overweight is a well-known risk factor for hypogonadism. Excess fat tissue can convert testosterone into estrogen, further lowering T levels. A sedentary lifestyle, poor diet, and excessive alcohol use can contribute indirectly. Conversely, vigorous exercise and weight loss tend to raise testosterone. (We’ll cover natural boosting later.)
Genetics and Developmental Issues: Some men are born with conditions that impair testosterone. For instance, Klinefelter syndrome (an extra X chromosome) leads to underdeveloped testicles and chronically low T. Undescended testicles (cryptorchidism) in infancy, if not corrected, can cause testicular failure.
Injury or Disease of the Testes: Direct problems with the testes (“primary hypogonadism”) reduce T production. Examples include mumps orchitis (mumps infection in adulthood damaging the testes), testicular injury or torsion, and testicular cancer treatments. Iron overload disorders (hemochromatosis) can also damage testicular tissue.
Pituitary or Hypothalamic Issues: The brain glands that drive testosterone (hypothalamus and pituitary) can malfunction (“secondary hypogonadism”). Pituitary tumors, radiation therapy to the brain, or genetic conditions like Kallmann syndrome (a developmental defect) can block the hormonal signals (LH and FSH) needed to stimulate the testes. Chronic pituitary disorders or high prolactin levels can likewise suppress testosterone.
Medications and Treatment Effects: Certain drugs or treatments can lower testosterone. Long-term steroid (cortisone) use or opioids can suppress the hormonal axis. Chemotherapy and radiation for cancer often temporarily (or permanently) reduce testicular function. Some prostate cancer treatments intentionally block testosterone.
Because multiple factors often coincide (for example, older age plus obesity), it can sometimes be hard to pinpoint the exact cause. A doctor will review your medical history, medications, and symptoms to identify likely causes.
In summary, low T in men is most often due to age and lifestyle-related health issues, while rare genetic or injury-related causes account for fewer cases.
How Testosterone is Tested
Diagnosing low testosterone begins with a blood test. Because testosterone levels naturally fluctuate throughout the day, labs typically require a morning blood draw (usually before 10 AM), when levels are at their peak. Your doctor will often order a total testosterone test as the first step.
Due to daily variability, it’s common for physicians to order two separate blood tests on different days to confirm consistently low levels. Research shows that in about 30% of men, an initially low testosterone reading returns to normal on repeat testing. This is why confirmation is essential before making any diagnosis.

